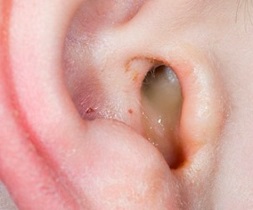
Ear Infections are common especially in children (due to a narrow ear canal and short eustachian tube), but can occur in adults too at any age. The ear has three sections – The outer, middle, and inner ear and ear infections commonly occur in the outer ear (otitis externa) or middle ear (otitis media). Inner ear infection (otitis interna) is rare.
OTITIS EXTERNA
Cause
The outer ear consists of the ear pinna and the ear (auditory canal) that ends at the eardrum (tympanic membrane). Otitis externa refers to an infection of the ear canal. The cause is generally water retention inside the ear canal which is a breeding ground for pathogens.
As swimming is one of the common causes, it is also called swimmer’s ear and occurs especially through improperly chlorinated or hygienic pools. However, it can also occur due to frequent long showers, irritant shampoos remaining in the ear, or injury to the ear canal lining due to frequent harsh ear cleaning, improper earphones/hearing aids, or intense itching (especially in those with eczema or other inflammatory skin conditions).
Most external ear infections are bacterial, while fungal infections may be seen in people with diabetes and reduced immunity. If the doctor suspects a fungal infection based on the history and appearance of ear discharge, a microbiological examination of the ear discharge sample may be conducted.
Signs and Symptoms
Symptoms include ear pain (otalgia), itching, feeling of fullness or heat in the ear, discharge (release of) of sticky fluid/pus (otorrhea), and a slight decrease or muffling of hearing, sometimes with a ringing sensation. On examination (usually done by an ENT specialist with an instrument called otoscope), there may be visible redness and swelling of the ear canal, with fluid.
Management
Most outer ear infections resolve spontaneously. Water should be kept out of the ear till the infection settles. Combination antibiotic -local anesthetic ear drops are often prescribed that help tackle the infection, and reduce the ear pain. These drops may be used 2-3 times a day for a week or so. Antifungal ear drops are given for fungal otitis externa (also called otomycosis). If needed an oral pain-killer may be given for the initial 1-2 days.
One should avoid head showering and swimming for at least 10 days, and on resuming use softball ear plugs if possible, and towel the hair and sides of the head thoroughly. A simple maneuver to remove retained water from the ear canal post swimming/showering is as follows: Make a cup of your palm on the ear, then tilt towards that side for 15-30 seconds pressing the palm cup to the ear. Thereafter remove your palm and pull that ear lobe down and remain tilted for another 15-30 seconds. Then dab out the excess water with a cotton ball placed at the entry of the ear canal. Repeat on the other side.
OTITIS MEDIA
Cause
Otitis media (OM) refers to infection of the middle ear, the space behind the eardrum (tympanic membrane) which contains the small ear bones that conduct sound. This part of the ear is connected to the throat by the eustachian tube and therefore can get infected when there is an infection of the throat (pharyngitis) or nose and sinuses (nasopharyngitis), so after a cold-cough episode. Common causes of infection are bacterial (Streptococcus, Pneumococcus, Hemophilus, Staphylococcus) or viral (flu virus, adenovirus, RSV, rhinovirus). A viral infection is often accompanied by secondary bacterial infection in otitis media.
Types of OM and Symptoms
A sudden onset of otitis media typically with fever, ear pain (otalgia), and muffling of hearing is called acute otitis media (AOM). Headache, cold and nasal stuffiness, cough, and malaise may also be present. Children present by constantly tugging at their ear and crying. There is usually pus buildup therefore it is also sometimes called acute suppurative otitis media (ASOM), and this can exert pressure on the eardrum sometimes rupturing it. In such cases, the person then gets pus discharge (release/coming out) from the ear. An acutely ruptured eardrum usually heals on its own and the reduction in hearing is temporary. AOM typically lasts 3-7 days and is always under 2 weeks.
Sometimes even after the acute infection and symptoms have resolved, fluid continues to build in the middle ear. This is called otitis media with effusion (OME) or serous otitis media. When this continues to happen repeatedly over a period of time usually 3 months or more, it is said to be chronic otitis media with effusion (COME). If this fluid turns into pus due to repeated infections, it is said to be chronic suppurative otitis media (CSOM). This is usually accompanied by a ruptured eardrum and ongoing ear discharge. A ruptured eardrum in CSOM takes long to heal on its own and can have more significant impact on hearing.
Complications
Rarely there may be complications in those with repeated suppurative otitis media like infection and damage of the mastoid, the bony protrusion behind the ear (mastoiditis), and spread to the membranes surrounding the brain (meningitis). Some of the important red flag signs of complications that need immediate medical attention are high nonresponsive fever, severe headache, dizziness, neck rigidity, red swollen ear that is painful to touch or move, facial pain, twitching of the facial muscles or paralysis of any part of the face.
Children with chronic otitis media can develop hearing and speech development issues.
Management
The doctor makes a diagnosis based on history and symptoms, and by performing a ear examination with an instrument called the otoscope.
Acute otitis media is managed with oral antibiotics given for 7-10 days. Supportive medicines include antihistamine-decongestant combinations, and anti-inflammatory-analgesics (NSAIDs) like ibuprofen, diclofenac, aceclofenac with paracetamol to manage pain and fever. Nose drops and sprays may be added when cold or sinusitis is present. AOM responds very well to treatment and usually resolves completely in 1-2 weeks, even if there is a perforation of the eardrum.
For chronic otitis media with effusion (serous), sometimes a procedure called a myringotomy (small hole in the eardrum) is performed and a tube is inserted that helps ventilate the middle ear and drain the fluid (tympanostomy tube). Such tubes may be removed after 12-18 months or may fall off on their own after resolution of the condition.
In the case of chronic suppurative otitis media, the patient is usually treated with antibiotic ear drops (or antibiotic-steroid combination drops). In some cases, courses of oral antibiotics may also be added. Periodic cleaning of the ear canal with antiseptic is also done by a health care assistant. Once the discharge stops, the person is followed up for 3 months to check the healing of the eardrum. If there is no spontaneous healing, a procedure called myringoplasty is performed where a graft is taken from behind the ear and patched on the damaged area of the eardrum. Sometimes a more extensive procedure called tympanoplasty may be needed, where along with the eardrum, additional repair of one of the middle ear bones may also be done.
OTITIS INTERNA
Cause
Otitis interna is an inflammation in the inner ear and is more commonly known as labyrinthitis or vestibular neuritis, as it affects the vestibular nerve supplying the labyrinth structure of the inner ear. It is far less common than otitis media and externa. The cause may be a viral or bacterial infection but is often not ascertained with certainty.
Symptoms
These include dizziness (vertigo), ringing in the ear (tinnitus), and loss of hearing. There may be nausea, vomiting, and loss of balance while walking.
Management
Treatment is symptomatic and may include antihistamines (like diphenhydramine, desloratadine, promethazine, cinnarizine etc), and corticosteroids like prednisolone. If bacterial infection is present or suspected then antibiotics may be prescribed.
The doctor will also explain some precautions for vertigo as avoiding sudden posture changes and movements and get up slowly from lying or sitting position. While experiencing vertigo, one should take the sitting down position, keep head still and avoid bright flashy lights. Physical therapists can teach exercises to help improve balance. Avoid driving till the labyrinthitis episode has resolved.
Labyrinthitis shows spontaneous resolution in 1-3 weeks. Though full recovery may take a few months, it usually does not recur.
Also read:
Common Cold and Flu- Know the difference, effective care and 10 alert signs