Diet for Diabetes should include the following simple 3-point approach-
1. Selection of Food Items:
a) Understanding Glycemic Index (GI) versus Glycemic Load (GL)
Glycemic Index (GI) measures how quickly a food raises blood sugar, while Glycemic Load (GL) accounts for both the speed of that rise (GI) and the total amount of carbohydrates (sugars) in a serving.
GI solely focuses on the speed of blood sugar impact with foods classified as low (55 or less), medium (56-69), or high (70-100).is a ranking from 0–100, whereas GL provides a more practical, real-life picture of blood sugar impact by factoring in portion or serving size, and total glycemic impact of a specific, realistic serving, calculated as GI multiplied by net carbs in grams in the serving divided by 100. Categories are low (10 or less), medium (11-19), or high (20 or more).
Green vegetables generally have low GI and GL and are ideal for diabetes and weight reduction.
Some fruits like watermelon have a high GI (about 75) because the sugar breaks down quickly. However, its GL is low-medium because a typical serving contains more water and less sugar. Similarly, a small potato has a high GI but a moderate-high GL, because the smaller amount of carbs/sugar per serving reduces the overall impact.
GI is useful for choosing better carbs, but GL is generally considered a better tool for meal planning and managing blood sugar, especially for diabetes. One should look up the GI of the food item, and calculate the GL in proportion to serving size and then make informed food choices. For high GI foods, one can reduce serving size appropriately.
The best way to choose items is to have a continuous glucose monitor (CGM) sensor in place for 1-2 weeks and understand the sugar responses to different food items and meals. For reference, given below are approximate GI and GL values for common food items and fruits. As mentioned, all green vegetables have low a GI,and GL.
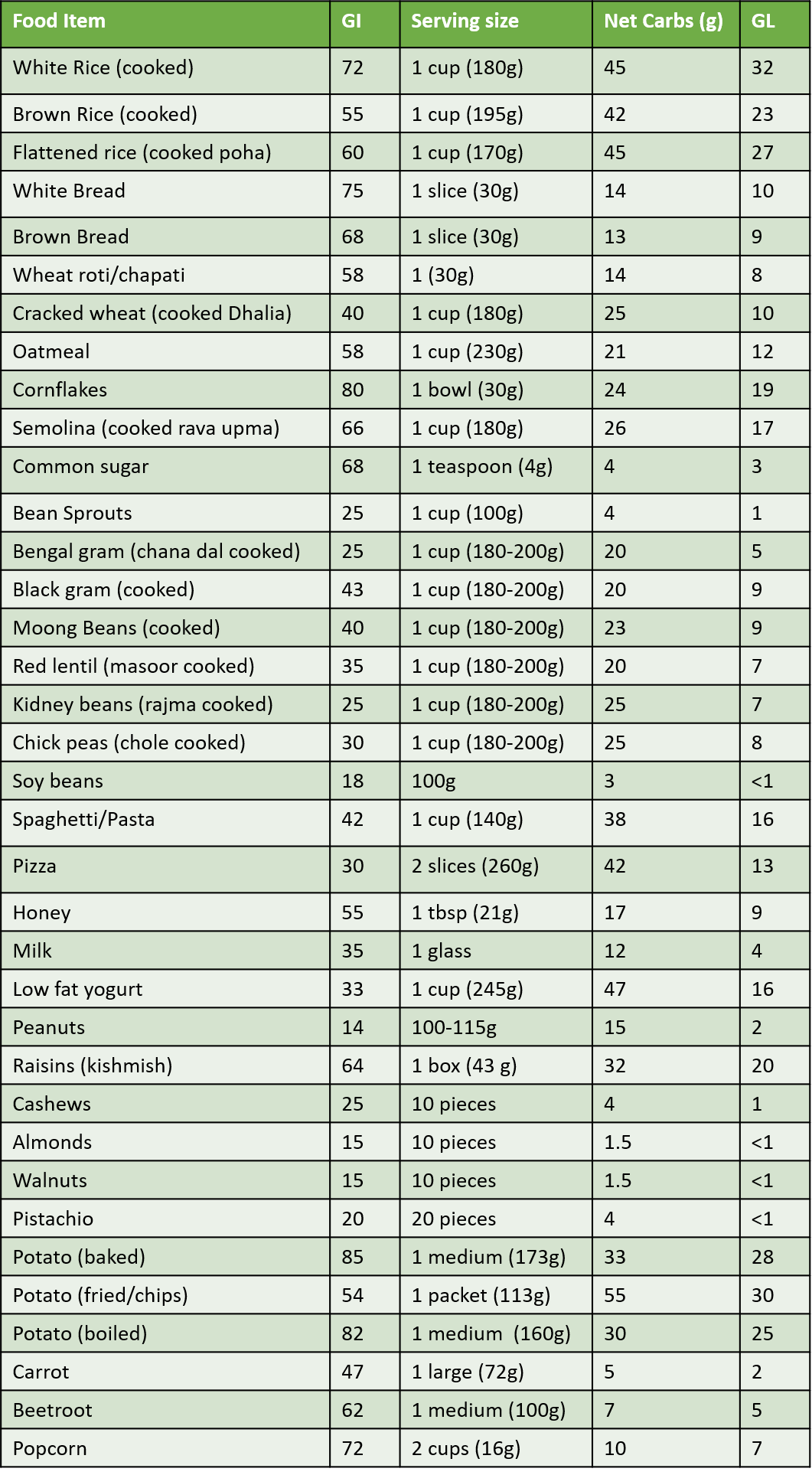
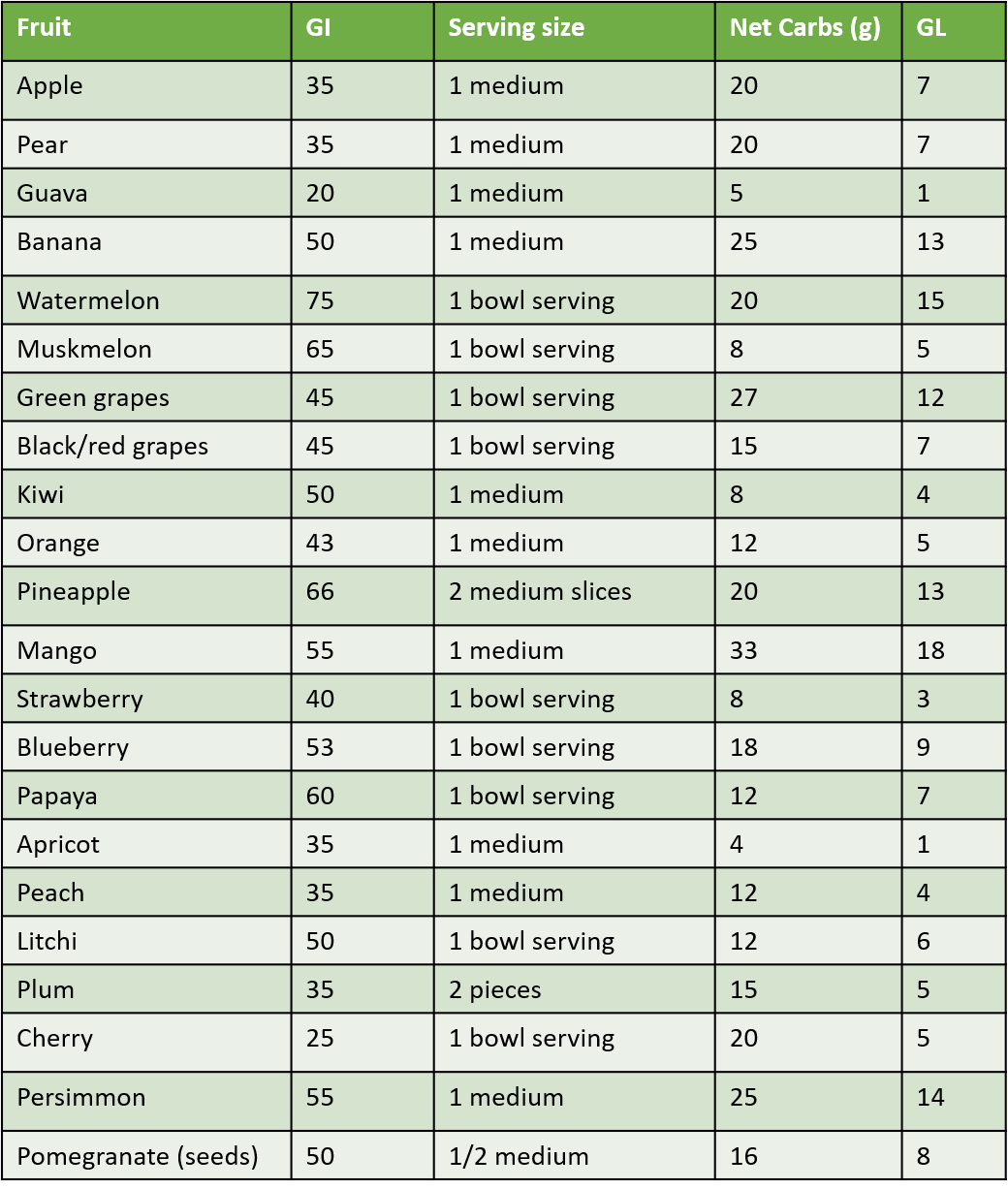


b) Selecting Cooking oil
Cooking oil and fat should include good fats – cis unsaturated fats along with some amount of specifically omega 3 fats and some amount of medium-chain saturated fats. Daily cooking oils can include oils like olive, sunflower, rice bran, or sesame. Coconut or palm oil can also be used 2-3 times a week. 2 teaspoons per person per day is the recommended measure while cooking.
2. Deciding the Proportion of Nutrients:
Your meal plate should be proportional as well as optimal in all nutrients:
- 1/2 plate with vegetables (all green vegetables, tomatoes and carrots).
- 1/4 plate with a starchy item like whole wheat (as roti/breads), brown rice, potato, corn, or any of the pulses (beans, peas or lentils).
- 1/4 plate with a protein item like lean meat, chicken, or egg. (vegetarian protein sources – paneer/tofu/cottage cheese, yogurt, soyabean, almonds). For vegetarians, pulses are a good source of protein as well as starch, so the plate can have 1/2 non-starchy vegetables, 3/8ths pulses, and 1/8th of a non-pulse protein source.
- Omega 3 fat sources should also be included in either lunch or dinner twice a week, like fish (salmon, tuna, herring, mackerel, trout) in the 1/4 protein component. (Vegetarians can cook in canola, soyabean, flaxseed oils or take walnuts twice/week).
- Include at least one fruit daily as a snack or part of the vegetable half of your meal plate.
- Include one unsweetened beverage and at least 1.5-2 liters of water in your daily diet plan.



The above plate distribution assures the appropriate glycemic index of food, balanced nutrition as well as adequate fiber. One should ideally design one’s diet with the help of the diabetologist and nutritionist who take into account the personalized glycemic response (PGR) of various foods.
3. Meal timings and frequency
- Timely meals are important.
- If the gap between meals is more than 3-4 hours, have a healthy mid-snack like a whole grain cracker, a fruit, nuts/avocados, yogurt, low-fat non-fried items, or buttermilk. A similar snack can be had at bedtime if the gap between dinner and bedtime is more than 3 hours.
- Meals should not be unduly delayed or skipped. Do not eat very heavily in any single meal.
One should ideally design one’s diet with the help of the diabetologist and nutritionist who take into account the personalized glycemic response (PGR) of various foods. Personalized glycemic response (PGR) refers to differences in postprandial (post-meal) rise in blood sugar between two people after consumption of the same food.
Medicines should be taken in strict accordance with dose, frequency, and relation with meals as prescribed. Doses should not be skipped or changed on one’s own.
Further Reading –
Diabetes: Understanding health risks, treatment, and taking effective diet-lifestyle measures
Incorporating the DASH diet to reduce BP, BMI and Cardiovascular risk

