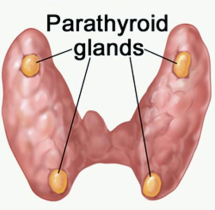
PARATHYROID HORMONE (PTH) FUNCTION
PTH is released from the parathyroid glands, which are tiny, pea-sized endocrine glands (4 or sometimes more) located behind the thyroid gland in the neck. PTH regulates blood calcium and phosphate like a sensor. Its main role is to increase blood calcium, especially when the blood calcium level fall so as to maintain a constant level.
PTH acts by –
- Increasing calcium absorption from the gut
- Increasing calcium reabsorption from the kidneys (decreasing calcium loss in urine)
- Increasing release of calcium and phosphate from bones by breakdown and remodelling, by direct inhibition of osteoblasts (bone-forming cells) and indirect activation of osteoclasts (bone breakdown cells).
- Decreasing blood phosphate levels by increased urinary phosphate excretion. (While PTH increases phosphate release from bone along with calcium, its action of increasing phosphate excretion is far stronger, causing a net decrease in blood phosphate).
REGULATION OF CALCIUM IN THE BODY
Along with PTH, two other hormones are also involved in blood calcium and phosphate regulation.
Vitamin D as its active form (calcitriol), formed in the kidney, also performs action 1 and 2 above, but counteracts action 3 and 4 of PTH. The main action of vitamin D is to ensure adequate calcium and phosphate uptake by the bones and maintaining bone mass. PTH increases the activation of vitamin D by stimulating the enzyme 1-alpha-hydroxylase that performs the final step of vitamin D activation in the kidneys.
Calcitonin, released by the thyroid gland, counteracts action 1, 2, and 3 of PTH, but co-performs action 4. Its main role is to decrease blood calcium, especially when calcium levels are high, when it promotes calcium and phosphate uptake by bones, and calcium and phosphate loss in urine.
Therefore, from the point of view of bone, PTH favors bone loss and calcium release into blood, while calcitonin and vitamin D favor bone formation and deposition of calcium and phosphorus in bone.
A normal total calcium level in adult blood is generally 8.5 to 10.5 mg/dL (2.12 to 2.62 mmol/L).
A more precise measure of active calcium is ionized calcium or “free” calcium, which gives an accurate estimate even if protein levels are low. This range is usually 4.6 to 5.3 mg/dL (1.16 to 1.31 mmol/L). Normal ranges can vary slightly between laboratories and age (younger adults or teenagers often have higher normal levels up to the mid-10s mg/dL compared to older adults
- High Blood Calcium (Hypercalcemia): Levels above 10.5 mg/dL
- Low Blood Calcium (Hypocalcemia): Levels below 8.5 mg/dL
HYPOCALCEMIA
Hypocalcemia, or low blood calcium, is primarily caused when there is low PTH due to under-functioning parathyroid glands (hypoparathyroidism), or due to certain drugs, including bisphosphonates (used for bone density), some anticonvulsants, cinacalcet, proton pump inhibitors, and corticosteroids.
Primary Hypoparathyroidism
This can occur due to surgical removal of the parathyroid glands during thyroid gland removal (thyroidectomy), genetic deficiency, severe magnesium deficiency, or damage due to tumors or radiation. Since low amounts of PTH are available, blood calcium falls. In such cases, lab tests reveal low blood calcium and PTH, and high phosphate levels, with low or normal vitamin D levels.
Hypocalcemia Symptoms:
- Tingling and Numbness: Frequently felt in the lips, tongue, fingers, and feet.
- Muscle Spasms/Tetany: Cramping in hands, feet, or legs, and severe, involuntary muscle contractions or facial twitching.
- Weakness and Fatigue
- Irritability, anxiety, confusion, memory loss, or seizures.
- Arrhythmias (irregular heartbeat).
- Dry-scaly skin, coarse hair, and brittle nails.
Treatment:
Acute hypocacemia treatment involves restoring calcium levels. Emergency treatment of acute or symptomatic Hypocalcemia includes IV Calcium Gluconate, magnesium supplementation, and clinical monitoring of calcium levels. If phosphate levels are very high, dialysis may be needed.
Chronic hypocalcemia treatment includes oral calcium and vitamin D supplements (calcitriol), and hormonal therapy with synthetic parathyroid hormone (PTH). Phosphate binder medicines are also available for the initial reduction of high blood phosphate.
Secondary Hyperparathyroidism
Vitamin D deficiency or low blood vitamin D3 can also cause low calcium levels, as the absorption of calcium from the gut falls. In kidney failure or chronic kidney disease (CKD), the activation of vitamin D cannot occur, so calcitriol (active vitamin D3) is low even if blood vitamin D levels are normal, causing calcium levels to fall. However, in such situations, the parathyroid gland senses low calcium and therefore starts to increase PTH release (secondary hyperparathyroidism).
Lab tests may show blood calcium to be low or normal, but PTH will be high. If the cause is kidney failure, phosphate levels may be high, and that in turn may further increase PTH release. Since we do not measure the active form of vitamin D in blood, in such cases, despite deficient vitamin D action, the levels of vitamin D3 in blood may be normal.
Symptoms:
Many individuals do not have symptoms initially. When they occur, symptoms often relate to bone loss (osteopenia and osteoporosis), like pain or tenderness in bones and joints, increased risk of fractures due to reduced bone density, kidney stones, and general weakness.
Secondary hyperparathyroidism can lead to the maintenance of blood calcium levels, but is accompanied by bone loss due to excess PTH.
Treatment:
Treatment consists of giving active vitamin D (calcitriol) or other vitamin D analogs, calcimimetics to reduce excess PTH secretion, and drugs to manage bone loss and osteoporosis. As the kidney is the most likely cause in many of these cases, managing the chronic kidney failure is the cornerstone of therapy.
HYPERCALCEMIA
Hypercalcemia is a condition characterized by excessively high calcium levels in the blood, often caused by overactive parathyroid glands (primary hyperparathyroidism). The most common cause is one or more parathyroid glands being overactive, usually due to a noncancerous tumor. In such cases, both blood calcium and PTH will be high.
High blood calcium can occur due to cancers like those of the lung and breast, and multiple myeloma, which cause high calcium, often when cancer spreads to the bones, leading to bone loss and calcium release in the blood. In such cases, while blood calcium is high, that may cause feed-back suppression of the parathyroid gland, and PTH may be low (secondary hypoparathyroidism). Other causes include sarcoidosis, tuberculosis, certain medications (e.g., lithium, thiazide diuretics), and overdose of calcium or vitamin D supplements.
Hypercalcemia Symptoms:
Mild hypercalcemia may show no symptoms, but higher levels can present with:
- Nausea, vomiting, constipation, and poor appetite.
- Increased thirst and frequent urination.
- Muscle weakness, twitching, and bone pain.
- Irregular heartbeat (arrhythmia)
- Fatigue, confusion, and in severe cases, coma.
- If calcium loss from bones is the cause, osteoporosis and fractures can occur.
- Kidney stones
Treatment:
Treatment focuses on lowering blood calcium while addressing the root cause. Primary hyperparathyroidism is best treated with surgery (parathyroidectomy) to remove the overactive, tumorous gland(s), and reverse high calcium, bone loss, and symptoms. For milder, asymptomatic, non-surgical cases, meticulous monitoring and adequate hydration are the conservative approaches. Medications include calcimimetics (like cinacalcet) that reduce PTH over-secretion by mimicking calcium in the parathyroid gland, along with drugs to manage bone loss (bisphosphonates).
Also read:
Weak, Thinning Bones: Osteoporosis Risks and How to get Screened
Chronic Kidney Disease (CKD) – 5 Key Points of Understanding